Release date: 2017-02-10

About 5%-10% of hereditary-prone cancers are attributed to cancer genetic syndrome. Identifying patients with a predisposition to hereditary cancer has significant benefits for both patients and high-risk relatives. In addition, short-term and long-term management of cancer patients can also be individualized based on their genetic status. For example, patients with positive BRCA1 and BRCA2 genetic tests will influence surgical decision making and have a risk of rapid metastasis. In the long run, long-term survival management programs for cancer patients can include the risk of monitoring and preventing a second malignancy. In addition, predictive genetic testing of patient family members will allow for more accurate risk assessment and initiation of appropriate screening and prevention strategies.
Â
Family history is the key to identifying individuals at risk for cancer or increasing the risk of primary cancer. Any collection of family history of cancer should provide sufficient information to initially determine genetic predisposition to develop a management plan. The doctor's first collection of family history can raise suspicions about hereditary tumor syndrome, and the relationship between doctors and patients provides multiple opportunities for reassessing and updating family history, and further research is possible. This in turn drives changes in cancer screening programs. In addition, the rapid development of the field of hereditary oncology and the long-standing links between oncologists and cancer survivors provide opportunities to re-evaluate and identify newly defined cancer susceptibility genes for new patients who have previously undergone genetic testing. A generation of genetic testing will also apply to them.
Risk assessment of hereditary tumors is also increasingly focused on improving quality in providing genetic testing and counseling services. For example, the American Surgeon Cancer Council (CoC) requires cancer risk assessments for patients, and genetic counseling can be referred to genetics professionals to provide testing services to patients. In addition, the American Society of Clinical Oncology (ASCO) Oncology Quality Practice Initiative (QOPI) includes guidance on the collection and interpretation of family history of cancer and whether to conduct appropriate testing.
Â
ASCO has pioneered the guidance and education of identifying and managing individuals with a predisposition to hereditary tumors. In 1996, ASCO issued a policy statement on genetic testing for cancer susceptibility to promote the expansion of access to health care for high-risk patients and families and to enhance the quality of such care. The statement was updated in 2003 and 2010. In the past two decades, ASCO has developed two versions of the education program (ASCOCurriculum: CancerGenetics and Cancer Susceptibility Testing), and has held many seminars to promote more and more online education models ( http://university.asco .org/ ).
Complete family history & minimal family history
Â
Complete family history information needs to be combined with the patient's individual cancer history. The gold standard for family history of medical genetics collection is the comprehensive mapping of the three generations of pedigree. However, this mapping assessment requires a busy workload, so it is not possible to obtain pedigree information for each patient in the clinic. Another important consideration is that family history is the most accurate among close relatives and loses accuracy in distant relatives.
Â
In most cases, hereditary cancer syndrome manifests as autosomal dominant inheritance and high penetrance. In this context, the family history of cancer among close relatives is the most relevant. Taking into account the guidance of genetic risk assessment, the NCCN guidelines and the American College of Obstetricians and Gynecologists focus on the referral criteria for hereditary breast cancer and Lynch syndrome in primary and secondary relatives, although they may choose to include family history information for third-degree relatives. . But for some special individuals, the family history of cancer does not meet the criteria for hereditary cancer syndrome, but may require changes in cancer screening. For individuals with cancer (or individuals at risk of developing a second primary cancer), the risk estimate may be to use less family history information.
Â
In breast cancer, risks can be estimated using, for example, the Claus model, which includes primary and secondary family history information and age at which the cancer is diagnosed. And of colorectal cancer screening recommendations can be drawn from a family history of colorectal cancer. Therefore, the family history of cancer of primary and secondary relatives is usually sufficient to assess the risk of the patient as well as the risk of common cancer or the risk of developing a second primary cancer.
Â
The age at which relatives are diagnosed with cancer should also be assessed, as this factor will determine screening recommendations in the genetic risk assessment.
Â
The pedigree of the mother and father should be assessed separately. Even for gender-specific cancers such as breast and ovarian cancer, both the paternal and maternal lines need to be evaluated because autosomal dominant inheritance can be passed through the father or mother.
Â
ASCO recommends defining the minimum family history of cancer patients as a family history of cancer in primary and secondary relatives. First-degree relatives are parents, children and siblings. The second-degree relatives are grandparents, aunts/uncles, prostitutes/scorpions, grandchildren, half-brothers and half-brothers. For each cancer patient, the following should be recorded:
â—Types of primary cancer
â—Diagnostic age of each primary cancer
â— pedigree (mother and/or paternal)
Patients should also be asked if there is a known hereditary cancer syndrome, previous genetic tests, and any ethnic information that may be relevant. For example, individuals of Jewish descent (especially Ashkenazi Jews) have a higher background in BRCA1 . Therefore, patients with breast cancer and / or ovarian cancer should specifically ask if they have any Jewish descent on the mother or father side. If so, a lower test threshold should be used. The elements of the minimum family history collection are summarized in the table below, which will make the initial cancer risk assessment easier.

Family history information for cancer should be collected and assessed at the time of initial visit and should be reassessed periodically. The reassessment includes obtaining any new family history information from the patient, and the clinician reassessing the family history based on new medical information and technological advances. Reassessment is important because the family history of cancer changes significantly over time. Patients can also learn more about their family history information, and once they have surpassed the pressure of initial diagnosis, they can be more actively involved in collecting this information, and the conversations around their diagnosis will begin to occur in the family. The time at which patients and oncologists participate in decision making or planning is an appropriate time to reassess family history.
Â
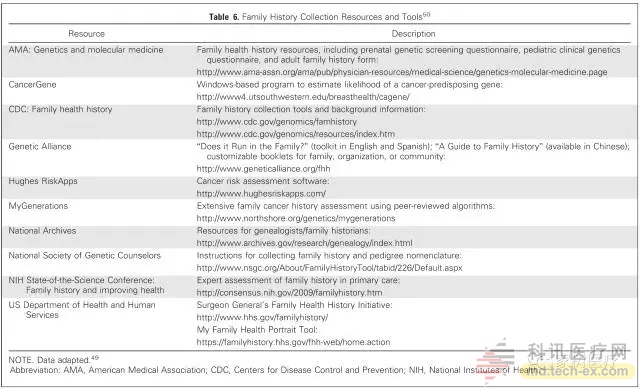
Family history should be interpreted based on the patient's personal cancer history, and this assessment should be documented and shared with the patient. Clinicians should identify a practical approach for cancer patients who need a more complete genetic risk assessment. Oncologists providing genetic testing should consider whether to provide additional genetic counseling and education. ASCO also provides some commonly used software systems for collecting family history, as shown below:
The manifestations of hereditary cancer include: early onset age of cancer, multiple cancer-affected relatives in the family, multiple primary tumors, especially in the same organ (eg, breast, colon or kidney). The latest research shows that individuals with specific tumor types should consider genetic testing regardless of family history.
references
1. Karen H. Lu et al. American Society of Clinical Oncology Expert Statement: Collection and Use of a Cancer Family History for Oncology Providers. J Clin Oncol 2014 Mar 10;32(8):833-40
Source: Jiashu Medical
Gummy Bear,Juicy Soft Candy,Juice Gummy Candy,Fruit Gummy Candy
Montreal Shantou Food Co., Ltd , https://www.montrealsnack.com