
Dr. Hannes Landmann, Sartorius Lab Instruments (Göttingen, Germany)
Dr. Kristin Menzel, Scientific Writer (Göttingen, Germany)
In 1908, Paul Ehrlich was inspired by the concept of "Zauberkugel", which for the first time theoretically described the assembly of toxic drugs onto so-called "nanocarriers". 1 Today, nanocarriers have many applications in modern medicine and biotechnology. A key application of these special nanomaterials is directed drug delivery, which acts as a pharmaceutically active transport module (ie, nanoparticles, vesicles, or micelles). 2, 3, 4, 5 It is speculated that this method is more effective and less toxic than the traditional method of administration. 6 In addition to drug delivery, other fields of application of nanocarriers have been developed over the past decades, such as magnetic resonance imaging or stem cell gene therapy using metal nanoparticles, 7 , 8 or optical imaging using quantum dots. 9
Nanocarriers can be classified according to their starting materials (ie, metals, lipids, polymers, and proteins) and post-production compositions (ie, vesicles, particles, and micelles). In general, the preparation of a nanoparticle suspension or vesicle dispersion in an aqueous medium involves three steps: a) nanocarrier assembly (eg by injection, thin film hydration or reverse phase evaporation), b) purification (eg chromatography) , dialysis or ultrafiltration) and c) concentration (eg ultrafiltration or evaporation).
This short review gives an example of some recent literature on the preparation of nanocarriers. It focuses on the concentration and purification step of using a different pore size (corresponding to a molecular weight cutoff (MWCO)) or a Sartorius Vivaspin ® by ultrafiltration device Vivaflow ® completed. The Vivaspin ® range ranges from 0.5 mL to 20 mL, while the Vivaflow ® system covers the range from 0.05 to 5 liters. As a result, Sartorius is able to handle sample volumes, membrane materials and MWCO ranges that are unmatched to meet the needs of different intended applications. Challenges in this area include buffer replacement after synthesis, desalting and cleaning 10,11 , removal of dissolved compounds 12, 13, 14 or aggregates. 15
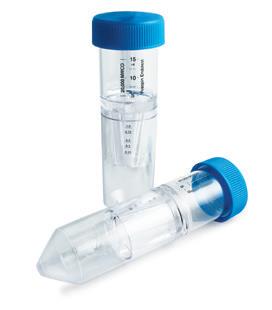
The purification process is important to achieve an isotonic state through purification, so as to avoid aggregation or agglomeration when applied in vivo, and to remove toxic drugs, ligands or other substances that may cause side effects. The importance of the concentration step is to modulate the amount of active ingredient in the drug to achieve the desired therapeutic or diagnostic effect.
Upon purification, the free material (starting material) is separated from the expected nanocarrier by size exclusion chromatography (SEC), which inevitably leads to product dilution and requires a subsequent concentration step. In contrast, diafiltration filtration does not result in significant dilution, but if a higher nanocarrier concentration is required, a concentration step is still required. Both separation methods require a large amount of expensive and time consuming manual operations. This disadvantage can be overcome by using Vivaspin ® centrifugal or peristaltic pump Vivaflow ® ultrafiltration system. The technology is low in cost, fast in operation, and has few manual operations. It is worth mentioning that the purification and concentration steps can be carried out simultaneously. 16
After purification of the nanocarrier, it is usually necessary to determine the drug loading (coupling or encapsulation efficiency). Coupling or encapsulation efficiency is a reference for the description and identification of nanocarriers. Other important properties include zeta potential and particle size distribution, which can be determined by photon correlation spectroscopy (PCS), high resolution transfer electron microscopy (HRTEM) imaging, or dynamic light scattering (DLS). The suspension or dispersion needs to be successfully purified and concentrated prior to performing these various assays.
The following table summarizes the literature on the purification and concentration of various nanocarriers using the ultrafiltration step. The table also guides you to how large the MWCO is.

Table 1 summarizes the application example using Sartorius Vivaspin ® or Vivaflow ® ultrafiltration nano carrier:
Nanocarriers: nanoparticles, vesicles, micelles | The particle size distribution is obtained by (HR) TEM or DLS , and the Z- average is obtained by PCS or other methods ( if reported ) | application |
Nanoparticles from metals, metal oxides and functionalized metals | ||
Iron oxide nanoparticles with a cisplatin-containing polymer coating | SD: 4.5 ± 0.9 nm (X-ray diffraction analysis) | Magnetic resonance imaging |
Functionalized iron oxide nanoparticles | SD: 38 and 40 nm (DLS method) | Stem cell gene therapy and tracking |
Gold nanoparticles | SD: 0.8 – 10.4 nm (atomic force microscopy) | Antibacterial activity |
Protein coated gold nanoparticles | SD: 15 and 80 nm (TEM method) | Drug delivery |
Functionalized gold nanoparticles | Core SD: 2 nm (TEM method) | Targeted imaging tools and antigen delivery |
Functionalized ruthenium nanoparticles | Z-average: 1.1 ± 0.6 nm and 4 – 14 nm | Diagnostic and therapeutic applications |
Functionalized nanocrystal | SD: 10 to 20 nm | Quantum dot imaging |
Nanoparticles from polymers, functionalized polymers and polymer vesicles | ||
Polymer nanoparticles | Drug delivery | |
Gelatin coated polymer nanoparticles | Z-average: 280 – 480 nm, depending on composition | Macrophage stimulating activity and drug delivery |
Docetaxel-carboxymethylcellulose polymer nanoparticles | Z-average: 118 ± 1.8 nm | Anticancer efficacy study |
Functionalized polymer vesicle | Z-average: 185 nm | Surface functionalization research |
Lipid nanoparticles and liposomes | ||
Liposomes and micelles | Z-average: liposome 100 nm, micelle 15 nm | Ischemia reperfusion injury |
Solid lipid nanoparticles | Z-average: 100 – 120 nm, depending on the lipid used | Drug delivery (brain targeting) |
Bacterial outer membrane vesicle | SD: 124 nm (TRPS method) | Adjustable Resistance Pulse Sensing (TRPS) Analysis |
Bacterial outer membrane vesicle | basic research | |
Bacterial outer membrane vesicle | SD: 95 nm | basic research |
Bacterial outer membrane vesicle | SD: 50 – 150 nm (TEM method) | basic research |
Liposomes | Drug delivery | |
Liposomes | Capsule hydrophilic drug (drug delivery) | |
Micellar | ||
Micellar | Drug delivery | |
Polymer-based hydrophobic drug micelle | SD (DLS method): 39 – 165 nm, depending on the compound used | Drug delivery |
Protein nanoparticle | ||
Protein nanoparticle | SD: 20 – 40 nm (DLS method) | Drug carrier research |
SD = particle size distribution
Sartorius ultrafiltration equipment | MWCO | Ultrafiltration purpose | reference literature |
Vivaspin ® 20 | 100 kDa | Purification and concentration steps | 7 |
Vivaspin ® 20 | 100 kDa | Cleaning step | 8 |
Vivaspin ® 20 | 5 kDa | Purification step | 17 |
Vivaspin ® 6 | 10 kDa | Separating nanoparticles | Dyes and cleaning | 18 |
Vivaspin ® | 10 kDa | Purification step | 19 |
Vivaspin ® | 5 kDa, 10 kDa | Purification and concentration | 20, 21 |
Vivaspin ® | 300 kDa and 50 kDa | (Before counting) Separation of quantum dot-antibody conjugates from the starting material | 9 |
Vivaspin ® | 30 kDa | Purification and concentration | twenty two |
Vivaspin ® 20 | 3 kDa | Cleaning | twenty three |
Vivaspin ® | 10 kDa | Concentration step | twenty four |
Vivaspin ® 20 | 10 kDa | Concentration step | 3 |
Vivaspin ® 20 | 100 kDa | Concentration step | 25 |
Vivaflow ® 50 | 100 kDa | Purification step | 26 |
Vivaflow ® 200 | 100 kDa | Buffer replacement and concentration steps | 27 |
Vivaspin ® 20 and 500 | 100 kDa | Buffer replacement and concentration steps | 28 |
Vivaflow ® 200 | 100 kDa | Buffer replacement and concentration steps | 29 |
Vivaspin ® | 100 kDa | Buffer replacement and concentration steps | 30 |
Vivaspin ® | 100 kDa | External buffer replacement | 2 |
Vivaflow ® 50 | 100 kDa | Remove free drug | 31 |
Vivaspin ® | 30 kDa | Separation of free material and concentration steps | 4 |
Vivaflow ® | Surfactant removal | 14 | |
Vivaspin ® 500 | 3 kDa | Separation of free drug from capsule drug (quantitative drug binding quantification by subsequent UV-visible analysis) | 32 |
references
1.Strebhardt, K & Ullrich, A:
Paul Ehrlich's magic bullet concept: 100 years of progress8, 473-480 (2008).
2. Jakoby, J.. Beuschlein, F., Mentz, S. Hantel, C. & Süss, R:
Liposomal doxorubicin for active targeting: Surface modification of the nanocarrier evaluated in vitro and in vivochallenges and prospects Oncotarget 6, (2015).
3. Klermund, L, Poschenrieder, S &t Castiglione, K:
Simple surface functionalization of polymersomes using non-antibacterial peptide anchors. J. Nanobiotechnology 14, 48 (2016).
4.Mulder, WJM et al..
Molecular imaging of macrophages in atherosclerotic plaques using bimodal PEG-micelles.
Magn. Reson. Med. 58,11641170 (2007).
5.Murthy.S. K:
Nanoparticles in modern medicine: state of the art and futurechallenges.
Int. J. Nanomedicine 2, 129-41 (2007).
6.Voigt, R. & Fahr, A:
Pharmazeutische Technologie für Studium und Beruf. Deutscher Apotheker Verlag.10th Edition 2010).
7.Unterweger, H. etal:
Development and characterization of magnetic iron oxide nanoparticles with a cisplatin-bearing polymer coating for targeted drug delivery. IntJ Nanomedicine93659- 3676 (2014).
8.Park, W.etal:
Multi-modal transfection agent based on monodispersemagnetic nanoparticles for stem cell gene delivery and tracking. Biomaterials 35, 72397247 (2014).
9.Chalmers, NI etal:
Use of quantum dot luminescent probes to achieve single cell resolution of human oral bacteria in biofilms. Appl. Environ. Microbiol. 73, 630- 636 (2007).
10.Hoffman, L W... Andersson, GG, Sharma, A., Clarke, SR & Voelcker, NH:
New insights into the structure of PAMAM dendrimer/goldnanoparticle nanocomposites. Langmuir 27, 6759-6767 (2011).
11. Rademacher, T. & Williams, P.: Nanoparticle-peptide compositions. (2014).
12. Allard, E. & Larpent, C: 24 Core shell type dually fluorescent polymer nanoparticles forratiometric pH-sensing. J. Polym. Sei. Part A Polym. Chem. 46, 62066213 (2008).
13. Prach, M.. Stone, V. & Proudfoot, L: Zinc oxide nanoparticles and monocytes: Impact of size, charge and solubility on activation status. Toxicol. Appl Pharmacol. 266, 19 -26 (2013).
14 Zhang, Y. etal: Therapeutic surfactant-stripped frozen micelles. Nat Commun, 11649 (2016).
15. Klasson, A. et al: Positive MRI contrast enhancement inTHP-1 cells with Gd2O3 nanoparticles. Contrast Media Mol. lmaging3.1061112008).
16.Simonoska Crcarevska, M. et al: Definition of formulation design space, in vitro bioactivity and in vivo biodistribution for hydrophilic drug loaded PLGA/PEOPPO-PEO nanoparticles using OFAT experiments.Eur.. J. Pharm. Sei. 49, 65- 80 (2013).
17.Boda, SK et al.: Cytotoxicity of Ultrasmall Gold Nanoparticles on Planktonicand Biofilm Encapsulated GramPositive Staphylococci. Small 1, 31833193 (2015).
18. Schäffler, M. et al: Blood protein coating of gold nanoparticles as potential tool for organ targeting. Biomaterials 35, 3455 3466 (2014).
19. Arosio, D. et al.: .Effective targeting of DC sign by a-fucosylamide functionalized gold nanoparticles. Bioconjug. Chem. 25, 2244-2251 (2014)
20. Miladi, l etal.: Biodistribution of ultra small gadolinium-based nanoparticlesas theranostic agent: application to brain tumors. J. Biomater. Appl.28, 38594 (2013).
21. Faure, ACetal Control of the in vivo biodistribution of hybrid nanoparticles with different poly(ethylene glycol) coatings. Small5, 2565-2575 (2009).
22. Benita, S., Debotton, N. & Goldstein, D.:
Nanoparticles for Targeted Delivery of Active Agent. (2008).
23. Tukulula, M. et al:
Curdlan-conjugated PLGA nanoparticles possess macrophagestimulant activity and drug delivery capabilities. Pharm. Res.32.27132726 (2015).
24.Ernsting. MJ, Tang, W. L, MacCallum, N W.&Li, S. D:
Preclinical pharmacokinetic, biodistribution and anticancerefficacy studies of a docetaxel-carboxymethycellunanoparticle in mouse mooels. Biomaterials 33,14451454 (2012).
25. Geelen, T., Paulis, L E., Coolen, BF, Nicolay, K & Strijkers, GJ:
Passive targeting of lipid-based nanoparticles to mousecardiac ischemia-reperfusion injury. Contrast Media Mol.Imaging8, 117-126 (2013).
26.Neves, AR, Queiroz, JF & Reis, S:
Brain-targeted delivery of resveratrol using solid lipid nanoparticles with functionalized with apolipoproteinEJNanobiotechnology 14, 27 (2016).
27. BogomoIny.E. et al:
Analysis of bacteria derived outer membrane vesicles usingtunable resistive pulse sensing. Prog. Biomed. Opt. Imaging =Proc. SPIE 9338, 4-9 (2015)
28.Blenkiron, C. etal..Uropathogenic Escherichia coli releases extracellular vesiclesthat are associated with RNA. PLoS One 11, 116 (2016).
29.Twu, O. etal Trichomonas vaginalis Exosomes Deliver Cargo to Host Cellsand Mediate Host: Parasite Interactions. PLoS Pathog.9, 2224 (2013).
30.Tong.TT. Mörgelin, M.. Forsgren, A. & Riesbeck, K.:
Haemophilus influenzae Survival during Complement-Mediated Attacks Is Promoted by Moraxeila catarrhalis OuterMembrane Vesicles. J. Infect. Dis. 195, 16611670 (2007).
31. Prado, JMD. Antoranz, JRC Barroeta, M.Ã.E.. Barroeta, BE & Diaz, MC: Liposomal formulations. (2009).
32.Achilli, E. etal..Preparation of protein nanoparticle by dynamic aggregation
And ionizing-induced crosslinking. Colloids SurfacesA
Physicochem. Eng. Asp. 486, 161171 (2015).
Salted Kelp Roots
The original ecological kelp means that we pack the young kelp with saturated salt water directly after washing without any preservatives.Original ecological products are the favourite of housewives.
Salted kelp:
How to eat:
- Soaking about 30 minutes to moderate salty
- Cook . make salad or add to hot pot after draining the wate

The difference between deep sea kelp and traditional ordinary kelp
Nutrational Effects
Salted Kelp Roots,Sea Kelp,Organic Kelp,Organic Kombu
Shandong Haizhibao Ocean Science and Technology Co.,Ltd. , https://www.haizhibaoseafood.com